2024 shook the US health market: cyberattacks, rising drug spend, and labor gaps exposed fragile systems and created urgency for change.
You’ll see why investors and leaders moved faster toward digital platforms, AI, and cloud partnerships after PwC and Deloitte reported rising costs and strong digital adoption plans.
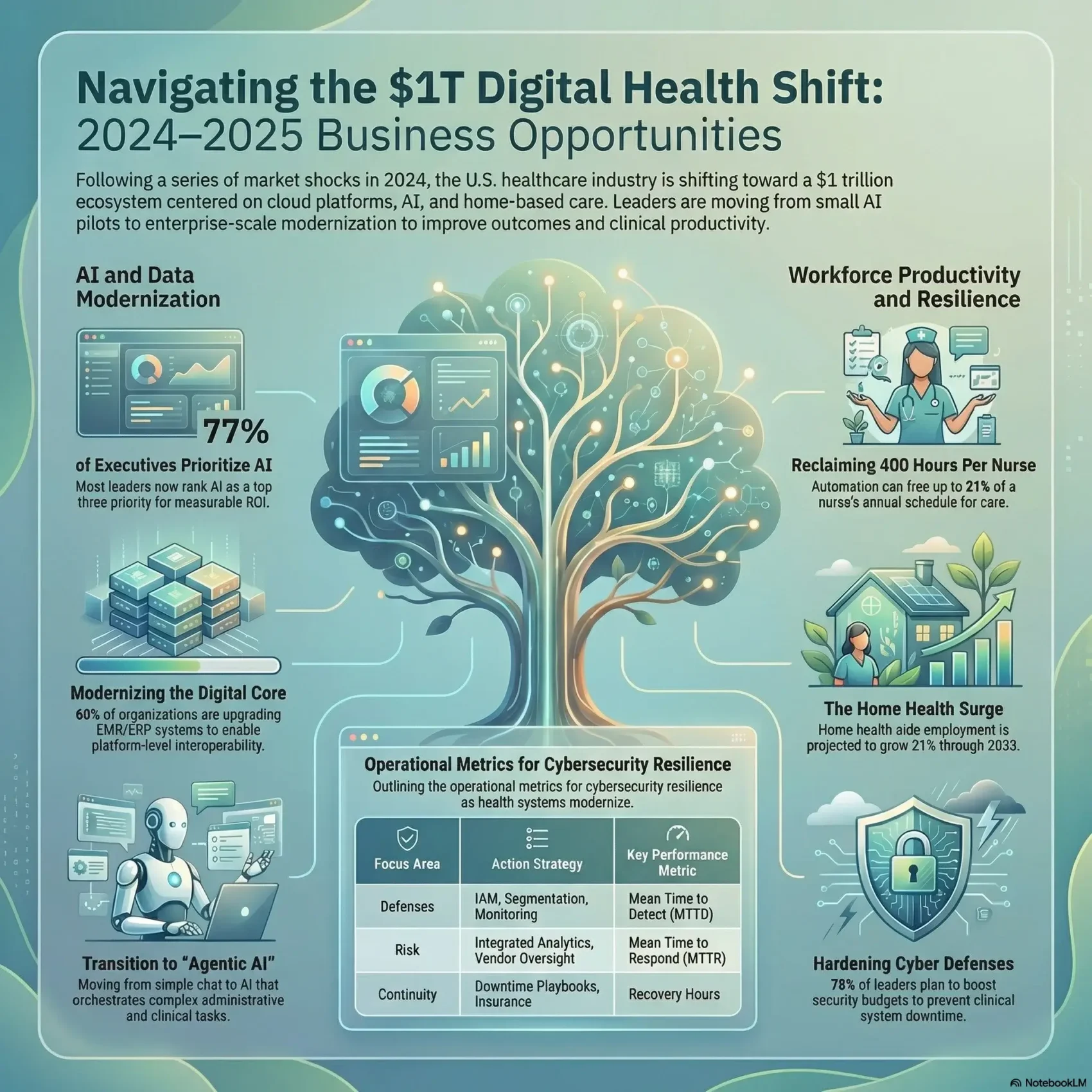
This moment opens clear opportunities for organizations that can modernize EMR and ERP, secure data, and deploy AI to improve health outcomes and reduce friction in care delivery.
The fight for affordability and consumer convenience makes payer and provider plays especially lucrative. Hyperscalers and AI innovators now sit at the center of a predicted $1T ecosystem shift.
Key Takeaways
- 2024 shocks accelerated demand for secure, data-driven care solutions.
- AI and cloud investments top executive agendas for measurable ROI.
- Modernizing EMR/ERP and interoperability unlocks scale and safety.
- Focus offers: payer affordability, provider productivity, and tech partnerships.
- Risk moves—cyber readiness and vendor oversight—are business enablers.
Why 2024-2025 Became a Pivotal Moment for Digital Health
A cascade of cost, policy, and climate shocks in 2024 forced health leaders to rethink digital priorities.
Macro forces converged: rising medical cost trends driven in part by GLP-1 utilization, tightened CMS reimbursement and STAR adjustments, DOJ deal scrutiny, major cyberattacks, and climate-driven disruptions. Together, these events exposed gaps in continuity, affordability, and data integrity.
From inflation and policy volatility to climate shocks
Cost inflation and benefit pressure shifted margins for payers and providers. CMS moves amplified the need for accurate information and faster data pipelines.
Extreme weather and system outages showed why remote monitoring and telecare matter for population resilience.
What stakeholders’ reactions signal about the next five years
Investor behavior is an early signal: Medicare‑aligned stocks outperformed, while Medicaid‑centric firms weakened. That pattern hints at policy-driven shifts and funding uncertainty.
- Expect more oversight and tighter affordability targets.
- Prioritize integrated benefit models to manage drug and pharmacy spend.
- Build data foundations that support quick responses to utilization spikes.
Translate this context into a clear operating model: balance near‑term performance with long‑term innovation so you protect access and improve outcomes.
HealthTech trends shaping the U.S. market right now
Higher drug demand and utilization shifted financial risk across the system. PwC flagged the biggest medical cost inflation in a decade, largely driven by GLP-1 uptake and specialty drug pipelines. Seven in ten consumers reported trouble affording rising health care bills, which forces urgent action on pricing and benefits.
Affordability tactics you can deploy include total cost of care management, site-of-care steering, and tighter pharmacy-medical integration. These measures help you control spend while keeping patients on effective treatment plans.
Utilization, margins, and practical levers
Provider volumes rose in 2024, but that increased utilization squeezed payer margins. You can rebalance risk with value-based contracts and targeted care pathways that align clinical goals with financial incentives.
- Improve STARs and risk adjustment by boosting coding accuracy and proactive outreach.
- Use real-time claims and care management data to spot utilization shifts early.
- Partner with specialty pharmacies and adherence platforms to bend the cost curve on chronic conditions.
Focus on transparent navigation and social risk data so vulnerable patients avoid cost-related nonadherence. Align clinical and financial KPIs to show measurable outcomes and preserve access while controlling cost.
AI and data: From pilots to platform-level value creation
AI investments are moving from small experiments to enterprise platforms that let you cut administrative cycles and improve clinical decisions. With 77% of health executives placing artificial intelligence among their top three priorities, your next move should be building a stable data foundation that scales.
Why leaders are prioritizing AI now
Executives see faster ROI when models run on modern EMR and ERP systems. About 70% plan digital platform investments and 60% target EMR/ERP upgrades to enable analytics and interoperability.
Modern data foundations and governance
Move past pilots by migrating to cloud platforms, enforcing lineage and access controls, and creating single-source information repositories. Strong governance protects privacy and ensures model quality so outputs support better outcomes.
Agentic AI and workflow automation
Agentic AI can orchestrate multi-step tasks—prior auths, denials management, scheduling, and documentation—so staff focus on complex care. Pair automation with human oversight to keep accuracy high.
Responsible AI and regulatory oversight
Track FDA updates on AI-enabled devices and the EU AI Act classification. Assess training data for bias, set monitoring rules, and require human-in-the-loop controls to meet compliance and protect care quality.
- Prioritize: EMR/ERP modernization and cloud migration.
- Define: high-yield use cases tied to operational KPIs and clinical outcomes.
- Educate: your teams on safe tool use and interpretation to sustain adoption.
Consumerization of care: Designing convenient, affordable, and personalized experiences
Consumers now expect health interactions to mirror retail apps: fast, clear, and tailored to their schedules. The 30% growth in ICHRA arrangements shows demand for choice and clearer pricing.
The AMA warns against one-size-fits-all consumerization because it can create new access gaps. Urban millennials and low-income single parents have very different needs. Telemedicine can cut work-related barriers for some patients but may miss clinical signals in others.
Building your digital front door and omnichannel engagement
Design a central front door that links scheduling, benefits, payments, and virtual visits across mobile and web. Use omnichannel messaging—SMS, chat, phone, email—based on patient preferences to lift show rates and adherence.
Personalization through analytics while avoiding one-size-fits-all pitfalls
Use data-driven segmentation to tailor outreach by demographics, language, and clinical risk. Incorporate social determinants information to meet people where they are.
- Balance convenience with clinical appropriateness across virtual, retail, and in-person settings.
- Clarify costs up front so patients choose the right site of care without surprise bills.
- Build feedback loops that turn experience signals and patient information into product improvements.
Governance and interoperability matter: ensure your solution architecture shares the full patient context and prevents bias as you scale consumer features.
Access and equity: Digital health without creating new deserts
Equity in digital care requires more than remote visits; it needs partnerships, protocols, and practical logistics that reach patients where they are.
Close gaps with fit-for-purpose models. Evaluate access barriers by geography and socioeconomic status. Design telehealth for follow-ups and straightforward conditions, and route first-time or complex cases to in-person care.
Closing gaps for rural and underserved populations
Build partnerships with community groups to tackle broadband, device, and cultural barriers. Offer mobile clinics or rotating on-site services as hybrid solutions.
When telehealth helps—and when an in-person visit is essential
Use short video consults to prevent missed work and improve timely access for low-income patients. Create protocols that flag when a hands-on exam is clinically necessary so convenience never overrides quality.
- Capture social and behavioral data to tailor outreach and navigation.
- Apply patient examples to guide triage and clear transitions between virtual and in-person care.
- Measure equity and outcomes to confirm your model expands access without creating new deserts.
Design for language access and accessibility across all digital channels. Embed continuous improvement so services evolve with community needs.
Policy shifts in Medicare and Medicaid: What they mean for your growth bets
Policy moves in Washington and at state capitols are reshaping how you plan Medicare and Medicaid growth.
Nearly 70 million Americans are on Medicare and about 90 million are on Medicaid/CHIP. CMS is tightening Medicare reimbursement and changing risk adjustment rules. That affects plan profitability and your growth math.
How to respond:
- Map likely Medicare reimbursement paths and stress-test your growth model under multiple rate scenarios.
- Evaluate state-level Medicaid exposure, including eligibility redeterminations and potential block grant or per capita cap structures.
- Use data to improve STARs and risk capture so you protect performance bonuses and clinical outcomes.
- Quantify margin sensitivity and build risk buffers into admin costs and network contracts.
- Plan scale moves—alliances, deals, or targeted exits—to keep competitive control in your market.
Prepare clear information packets for boards and investors that show scenario plans, timing tied to policy calendars, and state pilots where you can test innovations without undue exposure.
Pharma and PBMs: Transparency, rebates, and next-gen models under scrutiny
As specialty medicines and GLP‑1 costs swell, you face new rules and tougher questions about who benefits from rebates. Policymakers want clear drug‑level reporting and GPO revenue disclosure so plan sponsors can see true value.
- Rewrite contracts to tie fees to outcomes and total cost reductions rather than spread margins.
- Integrate pharmacy and medical data so utilization, adherence, and site‑of‑care decisions align with clinical goals.
- Adopt formulary innovations—value‑based contracts and guarantees—to balance access and affordability.
Strengthen governance and audit trails to withstand scrutiny. Build information flows that show employers real‑world outcomes for specialty treatment and quantify both financial and clinical impact.
Finally, partner with providers on coordinated pathways and invest in patient support solutions to cut abandonment and protect access while you control overall cost.
pharmacy integration can be a practical starting point to align incentives and demonstrate measurable value to plan sponsors.
Cybersecurity resilience: Preparing for inevitable disruption
When clinical systems go dark, your organization faces immediate safety and financial questions that demand tested plans. The US saw the highest number of major cyberattacks on health providers in 2024. Only about 15% of executives meaningfully measure financial cyber risk, even as 78% plan to boost cybersecurity in 2025.
First- and second-line defenses, integrated risk management, and vendor strategies
You’ll upgrade first- and second-line defenses from identity and access management to segmentation and continuous monitoring tailored to clinical systems.
Integrated risk management connects enterprise risk, cyber analytics, and incident response across business units and vendors. Rigorously assess cloud and third-party billing partners and embed contractual security obligations.
Quantifying financial exposure and stress-testing business continuity
Model downtime scenarios that include revenue cycle disruption, diversion costs, and fines. Stress-test mission-critical apps and define downtime workflows that protect patient safety and care continuity.
- Measure resilience KPIs (MTTD/MTTR, recovery time) and map them to clinical and financial outcomes.
- Run regular tabletop exercises with executives and clinical leaders to improve information sharing and decision speed.
- Ensure 24×7 coverage and defined escalation paths so teams engage within minutes, not hours.
| Focus | Action | Metric |
|---|---|---|
| Defenses | IAM, segmentation, monitoring | MTTD |
| Risk | Integrated analytics, vendor oversight | MTTR |
| Continuity | Downtime playbooks, insurance | Recovery hours |
Adopt secure-by-design for new technology and weigh cyber insurance or captive strategies against your quantified exposure. These steps give you control and help protect patient outcomes when disruption occurs.
Home health surge: Care moving closer to the patient
Delivering more services at home is changing how you staff, pay, and monitor clinical work every day.
Labor and funding signals favor expansion: employment for home health and personal care aides is projected to grow 21% from 2023 to 2033. You should build specialized labor pipelines and scheduling models that protect clinician well-being while meeting rising demand for care.
Labor outlook, reimbursement signals, and tech-enabled monitoring
Align with reimbursement paths that support hospital-at-home, SNF-at-home, and remote patient monitoring programs so episodes scale sustainably.
- Define clinical criteria and delivery protocols to keep care safe across home settings.
- Deploy technology kits—RPM devices and virtual nursing—so data flows back to care teams in real time.
- Redesign logistics for on-time supply, pharmacy, and durable equipment delivery to the patient’s door.
Opportunities include chronic care management and palliative services. Track market dynamics, quantify hours saved from avoided facility travel, and build payer partnerships with shared-savings models to prove value.
Workforce of the future: Productivity, retention, and well-being
Staffing pressure is no longer a distant warning—it’s changing how you design work in health care. Deloitte finds technology can free 13%–21% of nurses’ time, roughly 240–400 hours per nurse each year. That potential must be paired with workflow change so reclaimed hours translate into better care and less burnout.
Cut low‑value work to reclaim clinician time
Target documentation, referrals, and scheduling for automation so nurses and clinicians focus on patients. Use tech cautiously: automation should simplify tasks, not add new layers of work.
Upskill, redesign, and build trust
Invest in education and hands-on training so staff use AI and digital tools confidently. Pair learning with team-based roles and co-design to improve adoption and perceived value.
Enterprise strategies that stabilize costs and improve quality
Embed staffing analytics and flexible schedules to smooth peaks and reduce overtime. Link productivity gains to retention, cost stabilization, and measurable clinical outcomes.
| Focus | Action | Metric |
|---|---|---|
| Automation | Reduce admin tasks | Hours saved |
| Education | Upskill staff | Confidence scores |
| Workforce | Staffing analytics | Overtime hours |
Make this enterprise-led: govern workforce strategy across your tech roadmap and use workforce analytics to track progress and outcomes.
New value pools: Prevention, personalization, prediction, and point of care
Mapping new value pools helps you shift from reactive care to prevention-driven business models.
The PwC 4Ps—Prevention, Personalization, Prediction, Point of Care—give you a practical framework to improve outcomes and cut total cost of care.
Shifting business models to improve health outcomes and lower cost
Prevention means using clinical, behavioral, and social data to spot rising risk and intervene before problems worsen.
Personalization tailors treatment and outreach to genetics, behavior, and preference so patients adhere and feel seen.
Prediction uses AI to trigger early actions that reduce complications and avoid costly utilization.
Point of care brings services into homes and retail sites so access expands without sacrificing safety.
- Prove value with outcomes and cost metrics tied to chronic disease control.
- Run rapid pilots, scale when clinical and financial signals validate potential.
- Integrate pharmacist, behavioral health, and nutrition support into care pathways.
Design governance that ensures equitable access as you deploy technologies and new models. Align incentives with partners so savings from prevention and prediction are shared and sustained.
Deals and ecosystem plays: Where $1T in value is moving
A large transfer of market value is moving toward ecosystems built around cloud vendors, AI startups, and care-focused solution providers.
You should pick partners that accelerate your roadmap while lowering execution risk. Prioritize platform deals that de-risk modernization for claims, denials, and care coordination so you get measurable impact fast.
Partnering with hyperscalers, AI disruptors, and solution providers
Use a clear thesis for every deal: how it advances your model, reduces time-to-market, and protects differentiation. Structure JV or commercial agreements to share capabilities, data, and revenue fairly while protecting IP.
When you evaluate targets, demand information on security, compliance, and clinical validity. Map regulatory sensitivities like DOJ scrutiny and design compliant structures that can pass review.
- Align integration plans to your operating model so solutions scale across service lines and regions.
- Focus investments where the market is migrating—self-insured employers, virtual and at-home care, and automation layers.
- Set outcome-based SLAs that ensure value realization, not just technology delivery.
Finally, weigh build‑buy‑partner choices against speed, cost, and differentiation. Use due diligence and clear governance to turn ecosystem activity into practical opportunities for your organization.
Operating model modernization: From tech debt to scalable platforms
When you inventory tech debt and act, you convert maintenance drag into platforms that enable analytics, automation, and better care delivery.
Data interoperability, privacy, and measurable outcomes as table stakes
Start with a clear catalog: map legacy systems, custom builds, and manual workflows so you know where information is trapped.
Then consolidate onto scalable technology that supports APIs and standards so data flows across settings and partners without friction.
- Protect privacy-by-design: embed security controls and access policies before you enable cloud or AI use.
- Measure impact: define baselines and link platform investments to operational and clinical outcomes with transparent dashboards.
- Restructure roles: align product, data, engineering, and clinical owners to speed adoption and accountability.
“Interoperability and strong governance turn one-off projects into repeatable value across the organization.”
Finally, rationalize vendors, insist on configurable platforms for multiple care settings, and deploy change-management playbooks so frontline teams adopt new workflows quickly.
Go-to-market strategies: Turning trends into near-term opportunities
Designing buyer-specific offers makes it easier to prove value and win procurement cycles. Start with clear segmentation so each audience sees a tailored path from pilot to scale.
Segmented offerings for employers, payers, and health systems
Employers want transparency and cost control plus a better employee experience. Payers focus on utilization and admin efficiency. Providers need throughput and margin lift.
Build distinct value propositions that map to each buyer’s priorities and the common platform backbone you’ll reuse.
Validating ROI with evidence and real-world data
Use short, measurable pilots with clear success criteria — time-to-implement, workflow impact, and outcome improvements. Capture data fast and publish referenceable case studies.
- Align pricing to risk tolerance: shared savings, subscriptions, or guarantees.
- Pack implementation playbooks and integration accelerators to cut adoption friction.
- Arm sales with economic models, clinical evidence, and security information for faster due diligence.
“Validate ROI within a quarter when possible, then expand accounts by tracking outcomes and securing executive sponsorship.”
Conclusion
Leaders who focus on measurable wins—security, data, and simpler care—will capture the biggest opportunities ahead.
Turn volatility into momentum by modernizing platforms, scaling AI responsibly, and hardening cyber defenses so your health operations stay resilient. Prioritize actions that lift outcomes and affordability together, and choose partners that speed capability buildout without adding risk.
Double down on consumer design and workforce support to expand access and improve patient experience. Use data as your operating advantage, align Medicare and Medicaid plans to policy scenarios, and scale home- and point-of-care models where they clearly deliver value. Stay focused on the few ways that create the most impact now so your organization is future-ready and better at delivering sustainable health outcomes.
FAQ
What business opportunities should you prioritize in digital health for 2024–2025?
How did economic and climate factors make 2024–2025 pivotal for the industry?
Which market dynamics are shaping the U.S. health care landscape right now?
Why are so many executives prioritizing AI investments?
What must you do to build a modern data foundation?
How should you approach responsible AI and regulatory risk?
How can you design consumer-friendly care without compromising equity?
When is telehealth appropriate versus in-person care?
What do recent Medicare and Medicaid policy shifts mean for growth strategies?
How are pharma and PBM dynamics affecting digital health partners?
What should you do to strengthen cybersecurity resilience?
Why is home health growing and what tech supports it?
How can you address workforce shortages and burnout with technology?
Where are the new value pools in health care?
What partnership strategies unlock the largest deal opportunities?
What business opportunities should you prioritize in digital health for 2024–2025?
How did economic and climate factors make 2024–2025 pivotal for the industry?
Which market dynamics are shaping the U.S. health care landscape right now?
Why are so many executives prioritizing AI investments?
What must you do to build a modern data foundation?
How should you approach responsible AI and regulatory risk?
How can you design consumer-friendly care without compromising equity?
When is telehealth appropriate versus in-person care?
What do recent Medicare and Medicaid policy shifts mean for growth strategies?
How are pharma and PBM dynamics affecting digital health partners?
What should you do to strengthen cybersecurity resilience?
Why is home health growing and what tech supports it?
How can you address workforce shortages and burnout with technology?
Where are the new value pools in health care?
What partnership strategies unlock the largest deal opportunities?
FAQ
What business opportunities should you prioritize in digital health for 2024–2025?
Focus on solutions that reduce cost and improve outcomes: outpatient care delivery, remote monitoring, and medication affordability tools. Prioritize offerings that integrate with electronic medical records (EMRs), support cloud migration, and show clear return on investment for payers and health systems. Partnering with established cloud providers and analytics vendors helps accelerate adoption and demonstrate measurable value.
How did economic and climate factors make 2024–2025 pivotal for the industry?
Inflation, policy shifts, and climate-driven events increased pressure on budgets and supply chains, forcing you to rethink care models and resilience. Those stresses accelerated digital adoption as organizations sought efficiency, better data, and lower-cost care settings. Expect continued emphasis on cost control and operational agility over the next five years.
Which market dynamics are shaping the U.S. health care landscape right now?
Rising specialty drug demand (notably GLP-1s), affordability concerns, and shifting utilization patterns are changing margins for payers and providers. You’ll see payers negotiating differently with pharmacy benefit managers and providers exploring home-based and virtual care to manage total cost of care.
Why are so many executives prioritizing AI investments?
AI can streamline administrative tasks, support clinical decision-making, and unlock new revenue through prediction and personalization. When implemented on modern data foundations—clean EMR integration, strong governance, and cloud platforms—AI moves from pilots to scalable platforms that deliver operational and clinical impact.
What must you do to build a modern data foundation?
Upgrade legacy ERP/EMR integrations, adopt cloud-native architectures, and enforce data governance and interoperability standards. These steps reduce technical debt, enable analytics at scale, and make it easier to demonstrate outcomes and regulatory compliance.
How should you approach responsible AI and regulatory risk?
Adopt bias testing, transparent model documentation, and audit trails. Track FDA and EU guidance updates and embed clinical oversight into deployment workflows. This reduces legal and patient-safety risks while improving clinician trust.
How can you design consumer-friendly care without compromising equity?
Build an omnichannel digital front door that offers telehealth, in-person scheduling, and local community touchpoints. Personalize engagement using analytics but keep alternative, low-tech access for those with limited broadband or digital literacy to avoid creating new care deserts.
When is telehealth appropriate versus in-person care?
Use telehealth for routine follow-ups, chronic condition management, and behavioral health. Prioritize in-person visits for complex diagnostics, urgent procedures, and when physical exams are essential. Triage workflows and clear escalation paths help you choose appropriately.
What do recent Medicare and Medicaid policy shifts mean for growth strategies?
Changes in reimbursement and eligibility influence where you invest—value-based programs, home health expansion, and social-risk interventions often gain priority. Align your go-to-market plans with the new payment models and compliance requirements to capture upside.
How are pharma and PBM dynamics affecting digital health partners?
Increased transparency and rebate scrutiny push drug manufacturers and PBMs to align incentives with plan sponsors. You should offer solutions that demonstrate adherence, real-world evidence, and cost offsets that appeal to employers and payers.
What should you do to strengthen cybersecurity resilience?
Implement layered defenses, continuous monitoring, and vendor risk assessments. Quantify potential financial exposure and run business-continuity stress tests. Integrate security into procurement and incident response plans so disruptions don’t derail care delivery.
Why is home health growing and what tech supports it?
Aging populations, reimbursement shifts, and patient preference are moving care closer to home. Remote monitoring, point-of-care diagnostics, and mobile workflows help you scale home-based models while managing labor and reimbursement pressures.
How can you address workforce shortages and burnout with technology?
Automate repetitive admin tasks, standardize workflows, and use AI tools to free clinician time—studies show technology can reclaim substantial portions of nursing hours. Invest in upskilling, change management, and tools that build clinician trust to sustain improvements.
Where are the new value pools in health care?
Prevention, personalization, and point-of-care diagnostics are growing value areas. Offer predictive analytics, preventive care programs, and personalized interventions that lower total cost of care and improve outcomes for defined populations.
What partnership strategies unlock the largest deal opportunities?
Collaborate with hyperscalers, established EHR vendors, and specialized solution providers to access scale and distribution. Joint go-to-market agreements and data-sharing partnerships help you capture portions of the shifting
FAQ
What business opportunities should you prioritize in digital health for 2024–2025?
Focus on solutions that reduce cost and improve outcomes: outpatient care delivery, remote monitoring, and medication affordability tools. Prioritize offerings that integrate with electronic medical records (EMRs), support cloud migration, and show clear return on investment for payers and health systems. Partnering with established cloud providers and analytics vendors helps accelerate adoption and demonstrate measurable value.
How did economic and climate factors make 2024–2025 pivotal for the industry?
Inflation, policy shifts, and climate-driven events increased pressure on budgets and supply chains, forcing you to rethink care models and resilience. Those stresses accelerated digital adoption as organizations sought efficiency, better data, and lower-cost care settings. Expect continued emphasis on cost control and operational agility over the next five years.
Which market dynamics are shaping the U.S. health care landscape right now?
Rising specialty drug demand (notably GLP-1s), affordability concerns, and shifting utilization patterns are changing margins for payers and providers. You’ll see payers negotiating differently with pharmacy benefit managers and providers exploring home-based and virtual care to manage total cost of care.
Why are so many executives prioritizing AI investments?
AI can streamline administrative tasks, support clinical decision-making, and unlock new revenue through prediction and personalization. When implemented on modern data foundations—clean EMR integration, strong governance, and cloud platforms—AI moves from pilots to scalable platforms that deliver operational and clinical impact.
What must you do to build a modern data foundation?
Upgrade legacy ERP/EMR integrations, adopt cloud-native architectures, and enforce data governance and interoperability standards. These steps reduce technical debt, enable analytics at scale, and make it easier to demonstrate outcomes and regulatory compliance.
How should you approach responsible AI and regulatory risk?
Adopt bias testing, transparent model documentation, and audit trails. Track FDA and EU guidance updates and embed clinical oversight into deployment workflows. This reduces legal and patient-safety risks while improving clinician trust.
How can you design consumer-friendly care without compromising equity?
Build an omnichannel digital front door that offers telehealth, in-person scheduling, and local community touchpoints. Personalize engagement using analytics but keep alternative, low-tech access for those with limited broadband or digital literacy to avoid creating new care deserts.
When is telehealth appropriate versus in-person care?
Use telehealth for routine follow-ups, chronic condition management, and behavioral health. Prioritize in-person visits for complex diagnostics, urgent procedures, and when physical exams are essential. Triage workflows and clear escalation paths help you choose appropriately.
What do recent Medicare and Medicaid policy shifts mean for growth strategies?
Changes in reimbursement and eligibility influence where you invest—value-based programs, home health expansion, and social-risk interventions often gain priority. Align your go-to-market plans with the new payment models and compliance requirements to capture upside.
How are pharma and PBM dynamics affecting digital health partners?
Increased transparency and rebate scrutiny push drug manufacturers and PBMs to align incentives with plan sponsors. You should offer solutions that demonstrate adherence, real-world evidence, and cost offsets that appeal to employers and payers.
What should you do to strengthen cybersecurity resilience?
Implement layered defenses, continuous monitoring, and vendor risk assessments. Quantify potential financial exposure and run business-continuity stress tests. Integrate security into procurement and incident response plans so disruptions don’t derail care delivery.
Why is home health growing and what tech supports it?
Aging populations, reimbursement shifts, and patient preference are moving care closer to home. Remote monitoring, point-of-care diagnostics, and mobile workflows help you scale home-based models while managing labor and reimbursement pressures.
How can you address workforce shortages and burnout with technology?
Automate repetitive admin tasks, standardize workflows, and use AI tools to free clinician time—studies show technology can reclaim substantial portions of nursing hours. Invest in upskilling, change management, and tools that build clinician trust to sustain improvements.
Where are the new value pools in health care?
Prevention, personalization, and point-of-care diagnostics are growing value areas. Offer predictive analytics, preventive care programs, and personalized interventions that lower total cost of care and improve outcomes for defined populations.
What partnership strategies unlock the largest deal opportunities?
Collaborate with hyperscalers, established EHR vendors, and specialized solution providers to access scale and distribution. Joint go-to-market agreements and data-sharing partnerships help you capture portions of the shifting $1 trillion ecosystem value.
How should you modernize your operating model to scale?
Address technical debt, adopt interoperable standards, and measure outcomes tied to financial metrics. Privacy, data lineage, and measurable clinical impact are now table stakes for enterprise-scale platforms.
What go-to-market tactics work best for employers, payers, and health systems?
Segment your offerings and tailor value propositions: productivity and cost savings for employers, risk reduction for payers, and workflow integration for health systems. Validate ROI with real-world data and pilot programs that scale into long-term contracts.
trillion ecosystem value.
How should you modernize your operating model to scale?
Address technical debt, adopt interoperable standards, and measure outcomes tied to financial metrics. Privacy, data lineage, and measurable clinical impact are now table stakes for enterprise-scale platforms.
What go-to-market tactics work best for employers, payers, and health systems?
Segment your offerings and tailor value propositions: productivity and cost savings for employers, risk reduction for payers, and workflow integration for health systems. Validate ROI with real-world data and pilot programs that scale into long-term contracts.